The Truth Business Leaders Need to Face
A silent disruption of population health and human potential is causing a decline in economic growth and increased poverty worldwide. The number of citizens losing trust in leaders from public-private partnerships that ruled and mandated public health and climate policies and are responsible for eroding human capital is rising.
Recovery via improved investments is urgently needed. Creating healthy generations and rebuilding a flourishing economy both require trusted independent business leaders from small and medium enterprises (SMEs) who uphold finding truth and not doing harm as bedrock principles.
Human Capital is the Key Driver of Economic Growth and Poverty Reduction
Every business leader and politician knows that absence and poor mental health drain business.
The true problem business leaders need to face is the increase in unexpected deaths at all ages, a rise in frequent and long-term sick leave, and more people experiencing lifelong disabilities. Together, they lead to a considerable loss in productivity and high costs, a rise in bankruptcy of small and medium enterprises, and an increasing number of people in poverty.
Analysis of a Covid-19 Policy Score Card in the US shows a negative health effect for about 10% of the population and 30% of the civilian labor force. Business analysts are warning that this alarming negative trend is expected to continue over the next several years.
Moreover, those under 25 years of age, who will make up 90% of the prime-age workforce in 2050, experienced at critical moments in the lifecycle a derailing of developments by lockdowns and school closures. This amounted to a hidden but massive loss of unmet potential with a decline in lifetime earnings as high as $21 trillion globally.
The economic loss by the disastrous Covid-19 pandemic response and unneeded climate measures will exceed far beyond the $16 trillion virus. Soon, human capital will be the number one topic in risk management for business owners and investors for years to come.
Skyrocketing Sickness Hits the Heart of Business
Sickness hasn’t been this prevalent in decades. Independent investigators and insurance companies all point to similar observations, noticing a sharp decline in general health and well-being and an increase in sudden unexpected deaths of people in the workforce since 2021. According to Randstad 1.27 million employees miss work every day. The absenteeism rate rose to 6% in Q3 2023.
The growing number of people not able to work because of long-term illness is reflected in the economic data of many countries. Moreover, mental health problems among the youth have almost doubled.
Insurance companies in various EU countries, the UK, and the US have started to sound the alarm bell over the risk of recession and an increasing number of businesses that face bankruptcy due to high costs of human capital and poor performance.
Switzerland
Switzerland had a previous low sick leave rate of 2.4 days per year. This has changed. In the Swiss economy, absence from work due to mental illness has reached a record level and is 20% higher as compared to the previous year. Never have absences due to mental illness, burnout, post-traumatic stress syndrome, fatigue syndrome, or Long Covid syndrome been this high, with young people affected disproportionately. In the 18-24 age group, seven out of 10 people who are unable to work suffer from mental illness. This is four times higher than 25 years ago. These data reflect a structural trend.
A survey by AXA Insurance among SME found that almost two-thirds are confronted with absenteeism due to mental health issues. Workplace absenteeism weighs heavily on the activities of companies.
Extended employee absences can have detrimental consequences for the company’s operation. Among the most frequent repercussions are overtime and increased workload from the remaining staff (54%), costs related to recruiting additional personnel (38%), loss of production or failures in services (37%), and costs related to continuous salary payments.
Germany
Germany’s true economic disease, recession, includes rising sickness and declining productivity. In 2023 each employee had 19.4 days of sickness leave, almost equal to one month per employee and two times higher than in 2010. The highest increase was observed in 2022 and 2023. Filling open vacancies has become a headache for each business owner.
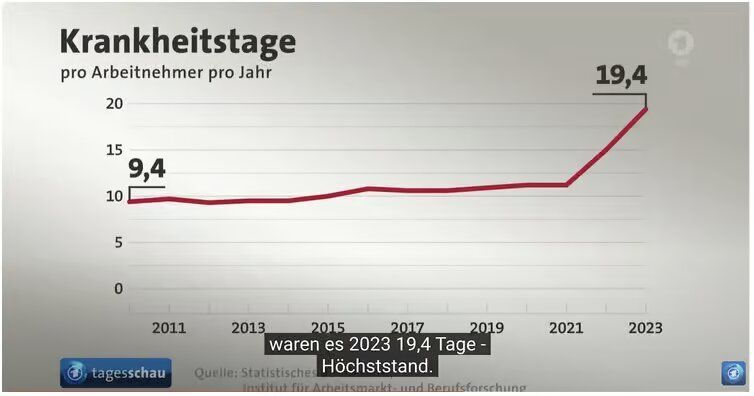
Source: tagesschau 20.00 uhr 26.01.2024
A recent study of the Kielerinstituts fur Weltwirtschaft observed that the increasing number of sick days cost the German economy between €27 billion and €42 billion per year. The number of sick days per employee increased from 8.5 days in 2020 to 11.3 in 2022 to 19.4 in 2023. The highest percentage of sick leaves is caused by respiratory diseases, followed by mental diseases (3.6 days/employee), and muscle disease and back pain (2.8 days/employee). In 2023 corona declined from 50% in 2022 to 34% of sick days.
According to AOK, absences due to mental illness have increased 48% since 2022, and this type of sick leave is associated with much longer periods of absence. In the study, a significant proportion in Germany complained that they were overburdened and stressed at work, with 78% complaining of exhaustion, anger, and annoyance, and 66% complaining of listlessness.
Remarkably, many young people between the ages of 18-29 years are more frequently sick than they used to be. One would expect this generation to be more resilient and with stronger immune systems. Some suggest they might stay home while still being fit enough to work. Unfortunately, a rise of mental health problems in Generation Z is seen in all countries evaluated in this article. Risk management should pay more attention to the unprecedented rise in mental problems in this age group.
UK
Although the UK has consistently been a strong performer internationally in terms of working-age participation, its post-pandemic rise in inactivity stands out. The UK is facing a recession due to unneeded pandemic and climate measures that eroded human capital. This is a hidden crisis that can no longer be ignored.
A recent report has found that workplace absences soared to the highest level in over a decade. It found stress to be a significant factor for both short- and long-term absence.
A staggering 2.6% of total working hours were lost in the UK last year, amounting to 18.6 million days off work and costing the UK economy £14 billion annually. UK employees are two whole days more absent than they were before the pandemic, with an average of 7.8 days per employee per year.
The number of people saying they are economically inactive due to long-term sickness is now 2.8 million (1.5 million women and 1.3 million men), an increase of more than 200,000 in the past year and 700,000 since the pandemic started in 2020. This is the number of working-age adults who are not at work or looking for jobs. Women are more likely to be in low-paid jobs and suffer the impact of austerity.
Analysis of trends in disabilities in Personal Independence Payments data by Phinance Technologies shows an upward trend for chronic and infectious diseases in most age groups.
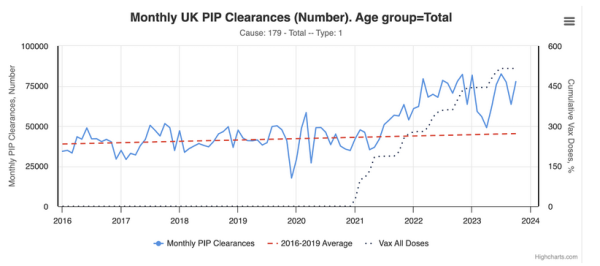
Moreover, the UK is facing significant problems in recruiting and retaining staff in the health and care sectors. Health reasons are increasingly a cause for staff to leave the NHS. The reported monthly sickness absence rate at NHS was 29% higher in 2022 than in 2019 (5.6% versus 4.3%). This equates to some 27 million days across 2022, which is on average 75,500 full-time equivalent staff, including 20,400 nurses and 2,900 doctors.
Reasons for NHS sickness absence are most prominently mental health problems. Mental health problems cost the UK economy £118 billion annually. This equals 5% of GDP.
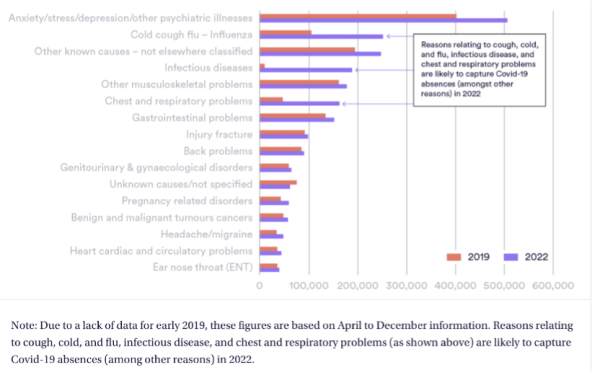
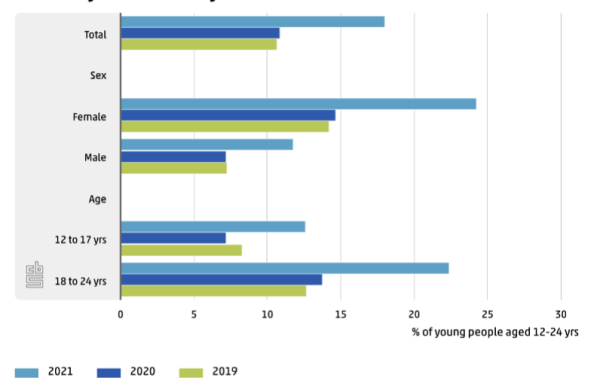
Reasons for sickness absences, average number of sick days per month 2019 and 2018
Also in other UK public sector groups, the sudden rise in sickness absence started in 2021.
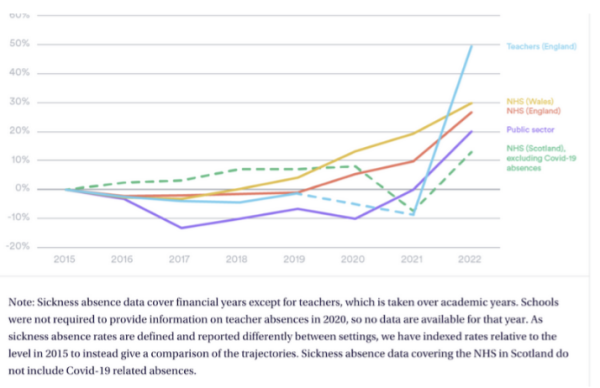
Changes to sickness absence rates across specified UK public sector groups (2015 baseline 28/6/23)
High absence levels and poor retention are both causes of and caused by increased pressure on services. The NHS risks getting stuck in a vicious cycle while 7.6 million people are on the waiting list for diagnosis and treatments. The NHS is putting patients at risk by letting 335 staff including doctors do their jobs from abroad.
Leaving people sick without diagnosis or with delayed diagnosis and treatments will result in higher healthcare expenditures and prevent employers and employees from engaging in other businesses, as they are stuck with high costs and are at risk for severe disease and even death.
Sickness absence rates are known to be related to season, infectious disease outbreaks, job satisfaction and employee engagement, workload over previous years, effort-reward imbalance, socioeconomic status, and gender. The latest report from the UK Health Security Agency shows that 70% of frontline healthcare workers refused the Covid-19 booster vaccine in 2023/2024.
In February 2024, hospitals experienced more pressure with three times more flu patients than last year. Primary care noticed a 9% increase in appointments in December 2023 as compared to pre-pandemic. Much of primary care is via e-health contact.
A continued weakness in productivity at work seen by most economists is the biggest long-term challenge to living standards in Britain. As shown in a recent study of health and well-being in Irish companies, workplaces are becoming more stressful with mental absenteeism rising.
Business is growing increasingly concerned about higher levels of inactivity and their economic impact on growth and inflation. Wages are rising because of skills shortages, which affect both employers and individuals. With more than 900,000 job vacancies and unemployment below 4%, the UK has a problem that won’t be solved without change.
The Netherlands
The Dutch insurance company Nationale Nederlanden calculated that in the year 2022, Dutch people were more frequently (1.5 times) and for more days sick (9 days/year) from work than ever before. From Q1 to Q4 2022, levels of sickness were increased compared to 2021 and 2020.
In 2022, the costs for the Dutch economy were €27 billion, €9 billion more than one year earlier. For the first time, the mean sickness percentage crossed 5%; in 2020, sickness percentage reached 4.7%, in 2021 4.9%, and in 2022 5.6%. Sickness percentage increased faster for women, being 1-2% higher as compared to men. Women were more frequently ill and for more days. The highest percentage of women at work is found in the Dutch healthcare sector, which is also the sector with the highest sickness rate. Analysis showed that low autonomy and high-stress level/pressure contribute significantly to absence, accounting for 2.9 million days of sick leave with mental health problems annually and costing €1 billion/year.
Recent investigations of the Dutch Trade Union Movement FNV reflected misbehavior at the Ministry of Healthcare and several other organizations in healthcare with employees feeling shut out, censored, and unsafe.
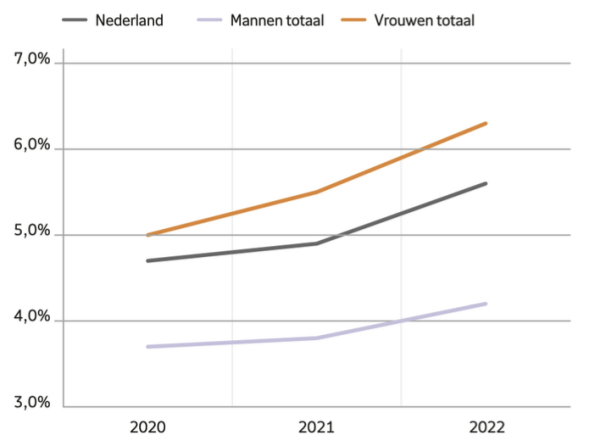
Percentage of illnesses 2020-2021-2022 men, women, and total
As in many other countries, mental health has worsened in the Netherlands at all ages from 2021 onwards, with the highest increase in ages 18-24 years and more for females than men. The number of young people who need to use invalidity benefits increased by 13% in 2021 and this trend is not going to reverse soon, as there is an expected increase of 30% per year for years to come.
In 2022 social security costs were €22.7 billion and are expected to rise to €1,8 billion in 2023. This is a skyrocketing increase as compared to 2022’s €93 million rise. The reason for this is still unclear.
Nearly half of the young people in the Netherlands are impacted negatively by the pandemic. The suicide rate of young people under the age of 30 in Amsterdam went up 40% in 2023.
Unfortunately, Dutch healthcare, as well as the Dutch Employee Insurance Agency (UWV) which is responsible for the invalidity benefit system, is facing a shortage of well-qualified employees. This has resulted in increasing waiting lists, holding sick people in uncertainty and desperation. In the worst-case scenario, young people are pushed into lifetime invalidity benefits due to insufficient time for accurate medical assessments.
As observed in a recent report by the ESB, the Netherlands is facing an ongoing trend in low productivity, far lower as compared to Switzerland, Denmark, and Sweden. The economic analysis thus far neglects to refer to the declining health status of the population. There is a rising number of people in poverty expected to reach 5.7% of the population in 2024. The authors of the report relate the decline in productivity to a transfer of high-productivity jobs to low-wage and low-productivity jobs and to more people starting to work as freelancers who are less productive as compared to large corporations.
In January 2024, a 60% increase in bankruptcy of small and medium enterprises as compared to the same month in the previous year was observed. The rising trend in bankruptcy started in 2022. Almost 25% of the healthcare providers (who report continuous sickness absence > 8%) in long-term care (especially those for people with disabilities) expect negative financial results at the end of this year.
Will the Netherlands be the next country facing recession?
US
For the general US population aged 16-64, from 2/2021 to 1/2022 the absolute numbers of the increase in disabled individuals amounted to about 1.460 million. Of those, 1.366 million were in the civilian labor force, and only 9.4% were not in the labor force.
A declining trend in absence rate was observed from 2002-2019 for both men and women. Increases started in 2020 (3.6%) and in the consecutive year, 2021(8.6%), and the largest rise occurred in 2022 (28.6 %). This was higher than the 2019 rate and a 50% rise in lost work time rates. Again, absence rates are higher for women than for men.

Absence rates 25-64 years old deviations from 2002-2019 trend
Like in many other countries, mental health in the US is a rising problem. Over 21% of the adults in the US experience mental health problems. This is 50 million Americans. On average 6% of youth (12-17 years) with major depression do not receive mental health services, and 55% of adults aged 18 and older did not receive treatment. Healthcare workers are receiving confidential mental health treatments.
In the US in 2021 and 2022, for the civilian labor workforce of 148 million, there was a 23% excess mortality relative to the expected baseline. In absolute numbers, this represents about 310,000 deaths. An estimated 1.36 million individuals aged 16-64 who are actively engaged in labor became disabled.
Even before the pandemic, 100 million people in the US who had a good paying job when they got ill now live with disability debt. Over 47% of persons with disabilities in the EU cannot pay their bills. The Human Rights report “Right to Work’ reveals the persistent gap in access to quality employment for persons with disabilities.
According to Edward Dowd, founder of Phinance Technologies, who posted on X the US Covid Policy Scorecard Human Cost for the year 2020: 458,000 all-cause excess deaths and zero excess disabilities from the trend. For the years 2021-2023 there are approximately 1.1 million all-cause excess deaths and 3.5 million excess disabilities from trend (population 16-64 years) and 28 million injuries with lost work time.
Rise in Disabilities Related to More Deaths
For the UK, Germany, and the Netherlands, excess deaths have been investigated by Phinance Technologies in the period 2020 to 2023 and others. Depending on the excess mortality methods used, the profile varies per age group.
Correlation analysis by Phinance Technologies showed quite a strong relation between the rise in disabilities and excess deaths for the US. An 84% rise in excess deaths was observed in the age group 25-44 years.
Dowd stated in an official roundtable in the US: ‘It is not possible to hide dead people.’ Dowd referred to One American CEO Scott Davidson, who revealed in a Chamber of Commerce meeting that he had seen 40% excess mortality for ages 25-64 years. More independent analysis in the US found an increase in sudden and unexpected deaths starting in 2021.
Governments in various countries have started to introduce new methodologies for modeling excess deaths. The ONS in the UK recently changed the methodology on excess death figures that modeled far fewer excess deaths in the past three years as compared to the previously used method. Even with these changes, there are still 11,000 excess deaths in 2023 and 43,500 in 2022 when Covid was only a minor player.
Moreover, the rising absence sickness, disabilities, and decline in productivity are another reflection on the decline in population health.
The increase is observed in all ages in the year 2021 when Covid-19 vaccines were rolled out, with the strongest signals in deaths and disabilities in the 15-44 age group with malignant neoplasm in the UK. The UK saw an unusual spike in middle age death (35-39, 40-44 years) in the first half year of 2023. According to a Bloomberg Intelligence Report, members of the public have been increasingly dying from heart failure, strokes, blood clots, and various forms of rapidly emerging cancers. If sustained, this could impact the pricing of all pension and life insurance companies.
Although a direct correlation has not been proven yet, in the past year more peer-reviewed studies have shown a risk for an increase in infectious diseases upon repeated injections with Covid-19 mRNA vaccines and an increased risk for adverse reactions.
A new peer-reviewed study that involved 99 million people over 8 countries identified potential links to conditions in the brain, the heart, and the immune system. Analysis of VAERS data on all vaccine deaths from 1988 to 2021 demonstrated that Covid vaccine deaths in 1 year are equivalent to deaths of 94 other vaccines in 33 years. More medical doctors started to question the safety and effectiveness of the Covid-19 vaccines in public.
UK MPs say that medicine regulators failed to flag Covid vaccine serious side effects. They believe that the Medicines and Healthcare Products Regulatory Agency (MHRA) was aware of heart and clotting issues in February 2021 but did nothing to highlight problems for several months. In 2022 Dr Maryanne Demasi published an investigative report in the British Medical Journal called ‘From FDA to MHRA are drug regulators for hire?’ calling for an independent drug and vaccine safety board. Will there be an inquiry into Covid vaccine safety soon?
Lockdowns, long-term wearing of facemasks, continuous stress and anxiety, and Covid-19 vaccines may all have contributed to the degradation of the human immune system. An increased risk of opportunistic pathogenic bacteria taking over a precious balanced immune system results in a systemic invasive bacteremia that may cause chronic diseases, acute respiratory distress syndrome, and sudden deaths.
The possibility that mRNA Covid-19 vaccines impair the immune system needs careful consideration per person. This is also why (repeated) vaccination could never be mandated or injected without informed consent. Moreover, a recent peer-reviewed article indicated that bivalent vaccines demonstrated moderate (29%) to negative efficacy. The association of increased risk with more prior vaccine doses was unexpected.
Recently, the FDA and CDC have confirmed that the Covid-19 vaccines do not prevent transmission of infection, so any mandates need to be stopped immediately and should be prevented forever. Mandates are unlawful under the Human Rights Act as was declared by the Supreme Court of Australia. Also in New Zealand, the Court of Appeal made a significant ruling that upheld a previous High Court Judgement that the Defence Force’s workplace Covid-19 vaccination mandates are unlawful. Moreover, the South Australian Employment Tribunal has ruled that employers are responsible for compensating employees who acquire vaccine injuries from work directives.
A Broken Society
Increasing uncertainties and pressure during the past four years have fueled fear and anger from various corners of society all over the world. The many protests from farmers to young doctors, supported by a growing number of citizens, are expressing how people feel. Being unheard of for well-based comments on unfeasible policies written behind desks and pushed into society as the only truth, low prices, effort-reward imbalances, and rising costs of food and energy are the main motivations for people to stand up for autonomy and freedom.
The whole population from children to elderly people is experiencing a dramatic degradation of the human immune system that can no longer be ignored.
Moreover, due to an overstressed and collapsing healthcare system, patients in many countries are facing increasingly long waiting lists for highly needed care. Quality and safety of healthcare are declining with more risk for misdiagnosis and unnecessary harm, with women and minorities most at risk.
At the same time, more children show permanent absenteeism from schools. In the OECD interim February Outlook ‘Strengthening the Foundation for Growth,’ it is stated that the impact of lockdown on children’s education during the Covid pandemic may have set economic growth 40 years back. Also, the immune system is less developed than it used to be, resulting in more children facing serious infectious diseases. In just three years, child mental health cases soared by 50%.
For elderly people, the availability of nursing home rooms and home care is becoming a huge problem due to the high sickness and retention rates in this sector. At the same time, there are more aging people now than before. Moreover, doctors, patients, and caregivers are confronted with a shortage in medical supportive materials and medicine, resulting in more emotional and often physical stress.
Care and education assistance are becoming a problem for family and community members. Voluntary unpaid work, most frequently delivered by women, is another responsibility that fills the priority list of the working-age population. This leaves them at increased risk for burnout, mental health problems, or other chronic diseases.
Moreover, the pandemic, climate measures, and a cost of living crisis have increased austerity and have driven an alarming number of people to the brink of poverty, even for healthcare employees in low-wage jobs with small contracts. Worldwide, policies have driven 70 million more people to extreme poverty. Malnutrition, undernutrition, and cold are the main drivers of severe disease and death, with increasing pressure on the exhausted healthcare and social system. This is a downward spiral that urgently needs a U-turn to save human capital.
Bridging the Divide
Tomorrow’s businesses that will survive the upcoming catastrophe worldwide will be led by trusted business leaders who understand that profit is a result of investments in human capital.
While alarming signals have been there for more than two years, many business leaders are neglecting their ‘gut’ feelings and are choosing continuous improvisations instead of working on a long-term strategy. The focus is short-term: a contract over the Green Deal, mergers and acquisitions, technology-based innovations, and/or moving business to low-wage countries with less absence and less stringent climate rules. They hoped times would turn for the better as soon as the pandemic was over.
In the end, there will be no escape: tomorrow’s C-suite risk management will shift the framework of each business leader to investments in creating belonging and employee health and well-being as a priority.
An increasing number of people are seeking a transformation for a healthy future. They prefer to work for companies led by supportive, transparent leadership. They seek a culture that stimulates interdependency and autonomy, where people dare to come forward and influence decision-making.
Leaders who love to guide uncertainties and rebuild societies will succeed. These leaders strive for open and respectful communication and do not avoid a dialogue on the effects of pandemic measures, climate-neutral policies, and the cost-of-living crisis. They take responsibility for mitigating the use of toxic words, stimulating free speech, bridging the divide, and creating belonging. They offer excellent salaries and stimulate eating natural nutritious food and a healthy lifestyle.
Moreover, it will be leaders who create opportunities to rehire former employees who have been excluded for choosing bodily autonomy and/or different well-argued opinions. They will support and invest in employees with disabilities via programs that will help them return to their own work and ensure that they are not shut out into low-wage jobs or unpaid voluntary work.
Author: dr. Carla Peeters
First published at Brownstone Institute
DR. CARLA PEETERS
Building transparent credible healthcare supporting healthy lives.
QUICK LINKS
SERVICES
All Rights Reserved | Carla Peeters


