Publicaties
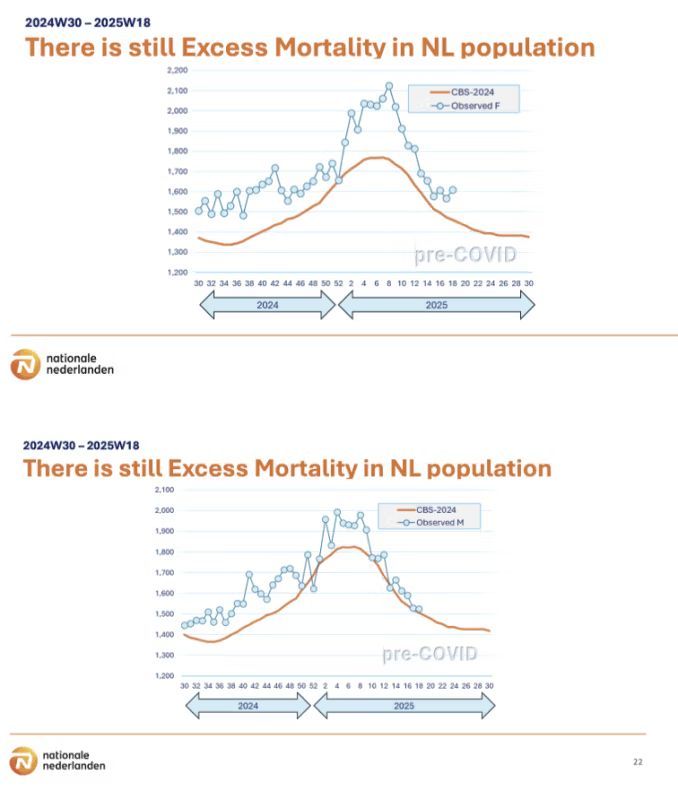
As women used to live longer than men even during severe famines and epidemics, a continued post-pandemic increase in female mortality and disabilities can’t stay hidden or neglected. During the Covid pandemic in many High-Income Countries, injuries, disabilities, and all-cause mortality started to rise above expectations. In 2020, the gender gap in mortality widened due to an observed increased mortality in men. While in 2021 male health seemed to bounce back to earlier trends, mortality and disabilities in women continue to rise above earlier trends and are not expected to solve themselves soon. This might cause a fundamental and permanent change in the dynamics of the gender mortality gap. Recent decisions on austerity measures for budgets on female health and welfare will exacerbate this hidden disaster. Instead, Public Health Experts and CEOs of insurance companies need to take their moral responsibility and turn to smart investments in female health, addressing all gender disparities, to reverse a downward spiral in global population health. A Sudden Rise in Excess Mortality and Disabilities In September 2024, Swiss Re published in their annual report, “Many countries worldwide still report elevated death in their population today.” This impact appears independent of healthcare system or population health. In the pessimistic model, Swiss Re would expect excess deaths to continue for another decade. There is also likely a degree of excess mortality underreporting. CFOs from other life insurance companies confirmed that experienced mortality rates are broadly in line with this report. A skyrocketing increase in disability claimants since 2020 is another puzzling factor why CEOs of insurance companies are facing major problems with their financial model. The growth in demand is much lower, and the number of people making claims is much higher than expected. Declining revenues may soon hit the corporate bottom line. For the first time in 80 years, the stocks from insurer Centene Medicaid plummeted in July 2025 by 41% after the insurer had to withdraw its full financial guidance because previous estimates were way off. The analysis from insurance companies is comparable with earlier reports from Phinance Technologies , which analyzed publicly available data from the US and UK using various methods. Other independent analysts observed similar trends. In recent years, hundreds of peer – reviewed articles discuss excess mortality and adverse events of special interest in various countries of pandemic measurements and after Covid-19 vaccinations. Boston University just published the all-cause mortality in the US as compared to other High-Income Countries and showed that excess death rates peaked in 2021 and declined in 2022 and 2023 but remained substantially higher than pre-pandemic rates, especially in the age group 25-44 years. Mortality among US adults aged 25-44 years was 2.6 times higher as compared to other High-Income Countries. A recent opinion from Kakeya et al. describes a significant increase in excess deaths after repeated Covid-19 vaccinations. Japan is the country with the highest per capita rate of messenger ribonucleic acid mRNA vaccination doses in the world. A systematic review on Covid-19 mechanisms of injury and death compiled with autopsy confirmation by a physician application suggests there is a likelihood of a causal link between Covid-19 vaccines and deaths. While there are studies that conclude there is no significant increase in stillbirths when women were vaccinated with the Covid-19 mRNA vaccine during pregnancy, a study based on VAERS data shows a significant increase. Another, not yet peer-reviewed, study indicates that Covid-19 vaccination with dose 1 during weeks 8-13 of pregnancy was associated with 3.9 fetal losses above expected for every 100 exposed pregnancies. A study in the Czech Republic on live births of vaccinated versus non-vaccinated women demonstrated a substantially lower successful conception rate among vaccinated women than for those who were not vaccinated. The fertility rate in the Czech Republic dropped from 1.85 births per 1,000 women in 2021 to 1.62 in 2022 and 1.45 in 2023. Births in the EU fell to 1.38 births per woman. Also the US reported a historically low birth rate in 2023. Many Western countries are facing a similar problem with dropping fertility rates as the health of young women declined during the pandemic and post-pandemic economic instability. Furthermore, maternal mortality rates accelerated at an alarming rate, especially from 2019-2022 in the US and UK, mainly caused by cardiovascular problems. The sharp spike in maternal death could not be explained by older age. Pregnancy-related maternal deaths are getting worse. In the UK, suicide remains the leading cause of direct maternal death in the first postnatal year. Pandemic measures resulted in a collapse of women’s health and income, especially for those with the lowest wages working in healthcare, social services, education, and retail. During this period, the number of female healthcare worker suicides and fatal overdoses increased . ‘When the health of those who look out for people’s health is at risk the whole population and economy are at risk.’ Furthermore, it is well known that women respond more strongly and may experience a higher risk for complications after vaccinations. An age and sex associated difference in immune cell population might explain this. Observations from vaccination trials in Guinea-Bissau suggest increased female-male mortality ratio associated with inactivated polio and diphtheria-tetanus-pertussis vaccine. There is precedent for the observation that infant girls experience increased mortality following receipt of vaccines. People in healthcare (80% women) have been recommended and sometimes mandated a yearly flu vaccine and several boosters with Covid vaccine. While not tested, a flu vaccine and Covid vaccine were mostly given at the same moment. A recent British study among 1,745 healthcare workers showed booster vaccinations did not contribute to the protection of the healthcare workforce in a post-pandemic setting. The Covid-19 vaccination may even temporarily increase the likelihood of symptomatic infection and workday loss. A study of a large cohort of 3805 healthcare workers in Sweden confirmed that adverse reactions after Covid 19 vaccination can lead to a substantial amount of missed work shifts that can cause organizational disturbances in staffing. Risks were found to differ by vaccine type and regimen used, age, and sex, with young female healthcare workers experiencing more adverse reactions. The recently published British and Swedish studies are in line with a few earlier studies. Recommending a combined use of four vaccines that prior to use had not been tested together during pregnancy when the immune system is following a precious time clock for the survival of both mother and child has been a risky approach. Clinical trials with the Covid mRNA vaccine during pregnancy have shown data with serious worries that should have been openly discussed with pregnant women. Moreover, long-term effects for both mother and child remain unknown. After the Netherlands and the UK, the US only recently said that Covid-19 vaccines are no longer recommended for healthy people under the age of 65 years and pregnant women. Whereas Covid-19 vaccines are still recommended for immunocompromised people, unfortunately they might be more at risk for experiencing Covid-19 infections after booster immunizations. Although a causal relation remains difficult, the effects of repeated mRNA vaccination in combination or shortly before or after other vaccinations and/or using (psychiatric) medicine need to be elucidated. Sex differences in cost-effective harm analysis will help future decision -making. Last week Robert F Kennedy, Jr stopped financing 500 million subsidiaries for the mRNA vaccine platform. Also the director of the NIH Dr Jay Bhattacharya wrote an opinion piece for the Washington Post: “Why the NIH is pivoting away from mRNA vaccines.” As a vaccine for a broad public use mRNA technology has failed to earn public trust. A Post-Pandemic Increase of Female Mortality In nearly all populations, women live longer than men. The ubiquity of female survival advantage for all ages, even during famine or epidemics, when mortality is extraordinarily high is changing. Unfortunately, there is limited information available on sex differences in excess mortality from major respiratory infectious diseases. A peer-reviewed study on the first wave of the Covid-19 pandemic in Italy observed that gender differences in excess risk of death existed, but with a nuanced and non-consistent picture. The general finding of this study is that males up to 75 have been suffering more excess deaths as compared to females. However, this picture is less clear-cut at older ages when more women are living in nursing homes which during the Covid pandemic showed the highest mortality rates. A study from the Netherlands on sex differences in Covid-19 mortalities skipped the data from healthcare workers and people living in nursing homes (mostly females) to confirm that male sex is a predisposing factor for severe Covid-19 independent of age and comorbidities. Some other studies and a recent study (preprint) suggest Covid-19 did not produce lasting shifts in pre-pandemic sex differences in mortality in High-Income Countries and did not change the fundamental dynamic of the sex mortality gap. The authors observed that the male disadvantage in the Covid-19 mortality based on absolute death counts was concentrated in the pre-vaccine phase and declined over time. Relative increases in mortality were often similar between sexes, and in some cases, greater among women. Another study on excess mortality of 561 regions and 21 countries in Europe indicate that in many European regions, where drops in life expectancy were more moderate, more pronounced life expectancy losses were found for women. The authors suggest that the degree of mortality deterioration is not necessarily linked to biological sex. A cohort study of the overall impact of the Covid-19 pandemic on mortality in France observed four consecutive years of excess mortality and a growing impact on people from 20-60s, particularly men. Unfortunately, no peer-reviewed publications on sex differences and excess mortality cover the years 2024-2025. Yet, during the International Conference of Actuaries in 2025 Nationale Nederlanden, a Dutch insurance company, presented a continued rise in female excess mortality in the Dutch population from 2024-2025, while male excess mortality tended to decline. Furthermore, analysis showed a much higher degree of female excess mortality as compared to EU countries in general, while the Dutch male population experienced a better life expectancy as compared to EU countries.
Many countries now face a growing problem with an aging population and declining childbirths. Too many infants still die unnecessarily before the age of five years. Countries increasingly struggle to keep their economies stable. While Public Health experts communicate to focus on healthier future generations, declining health in young females is ignored. The healthiest generation with a flourishing economy is achieved by a holistic strategy addressing Young Women’s Health as a Public Health priority. The Healthiest Generation of the World in 2040 A Federation of Organizations involved in Public Health in the Netherlands has the ambition to reach the healthiest generation of the world in 2040 . Health is aimed at all levels; mental, social, and physical. To achieve this goal, the Netherlands needs the healthiest young females of the world. In contrast, data analysis from the Netherlands shows the opposite; the health of young women is declining fast. In other Western countries, it won’t be much better. The health of young women has worsened worldwide; it is time to face reality. Women’s bodily functioning and metabolism differ from men and need specific female-adapted health support. While many health problems in a population could be prevented when young females are supported for optimal health prior to pregnancy, this is not a priority of Public Health Agencies. Good health for the next generation starts with a strong and resilient immune system before pregnancy and during the first 1,000 days around pregnancy, birth, and postpartum breastfeeding. Childbirth and children’s health are declining; the number of women dying during pregnancy (within 42 days after labor) is increasing, as well as the number of abortions. Without change, these conflicting trends may develop into a disaster touching all levels of society. The Public Health Future Outlook of the Netherlands predicts that close to 12 million people will have a chronic condition by 2050. Young Women’s Health Is Declining Around half of the young people aged 6-25 years in the Netherlands experience mental health problems. Moreover, 47% of the people aged 15-44 years are diagnosed with at least one chronic disease, with young women more often diagnosed than men. When diagnosed with a chronic disease, people work less, experience more sick leaves, and are less productive. Unfortunately, not being able to work contributes to poorer health and income. An even larger percentage of young people (79%) still suffer from a negative impact of the pandemic, with women and lower-educated individuals hit hardest and experiencing mental problems like emotional exhaustion, stress, and hyperactivity. A recent study published in PNAS showed a faster aging of the brains of young females as compared to young males, which might be related to chronic stress exposure. Students experience more stress than before due to worries about inflation and the high costs of living. Within the EU, the Netherlands has grown into the most expensive country to live in. Unfortunately, there is much more that is troubling the health of young females. Increased Drug Use and a Dangerous Beauty Myth During the pandemic, the use of antidepressants increased by 16% for those aged 16-24 years and for children. Women are prescribed antidepressants earlier and take them twice as much as men. While the positive effects of SSRI have been criticized repeatedly and women report more side effects than men, these medicines are still frequently prescribed by medical doctors. One in four young people in the Netherlands use Ritalin or Concerta ( methylphenidate ) without a medical prescription to improve concentration and study results. Most people are unaware of the potential risks, like sudden death, that are well-known as a potential side effect. Research has shown that 5.5-22.5% of the young have used ADHD medication without a doctor’s prescription. Furthermore, in mid-2023, a worrisome increase in NSAID like paracetamol (Tylenol or Acetaminophen) and ibuprofen use was observed, especially in young girls, increasing the risk for poisoning. The use of antibiotics like amoxicillin increased for children 0-10 years (55%) and for those aged 11-20 years with 50%. As 2023 was the first year after the pandemic with all festivals open to the public, an increased use of party drugs (like ecstasy ) among those aged 16-35 years was noticed with regularly registered symptoms of poisoning. The online and interconnected world exposes the risk of cyberbullying among young people. Ironically, many are feeling lonelier than ever before and are struggling with their weight and self-confidence, setting them up for poor health as adults. The beauty myth is another danger. During the years 2019-2022, the use of fillers increased by 80%, and the use of Botox doubled among young women. Exposure to microplastics, nanoplastics, and nanoparticles has increased. Furthermore, the concentration of PFAS/PFOA in Dutch drinking water is found to be above the norm and may decrease the fertility of both women and men. On the other hand, the use of oral hormonal contraceptives by young girls diminished in the Netherlands, with only a slight increase in the use of an intrauterine hormonal device. Recent studies showed that there is an increased risk, although small, of myocardial infarction or stroke when using hormonal contraceptives. The use of an intrauterine device with levonorgestrel did not show the risk. Given the extensive and ongoing reliance of millions of young women on these drugs, ensuring their safety remains a critical responsibility of the medical community. As well as medical doctors informing young women of potential harm based on the latest scientific literature by informed consent. Over the past 4 years, girls and young women have been exposed to repeated HPV vaccinations and Covid-19 mRNA vaccines within a short period of time, for both of which side effects in women have been reported to be more frequent and severe. Possible interactions and/or interference with these vaccines and long-term effects on the immune system and microbiome have not been investigated beforehand. Neither was knowledge available when it started in 2021 on the possible risks and short- and long-term effects when four vaccines before 22 weeks of pregnancy were introduced. Nutritious Food Not Affordable for Many The importance of daily consumption, as recommended by the WHO, of 400 grams of fresh fruit and vegetables, meat, milk products, and eggs for a healthy life and joyful social and working life is unknown by many young people. For most of them, it has become unaffordable . (Ultra)processed foods are the cheapest satisfying foods with a well-designed composition of low-cost ingredients, sugar, fat, and salt that change the microbiome. Home, school, commercials, social media, influencers, mobile phones, and retail environments are driving obesity and being overweight in children and adolescents, often concurrent with undernutrition and anemia. A growing body of evidence shows that the billions of microorganisms present in our body are intimately involved in weight gain and loss and immune training and modulation, as well as overall host homeostasis. Around 33% of the population in the Netherlands does not consume fruit and vegetables daily. As of 2024, 7.1% of Dutch children live in poverty, and this number is still growing . More children might be undernourished, which is associated with impaired growth, neurodevelopment, and increased infectious morbidity and mortality. To reverse the problem of malnutrition, the delivery of free meals has recently started at primary schools. Unfortunately, this does not make a difference for the children at secondary schools. While sending funding to developing countries to prevent malnutrition, a similar problem appears in front of our eyes in the Netherlands. The young generation predominantly eats more plant-based foods, as it would improve climate change. Almost 30% of young women prefer to shop for vegetarian food, and 0.7% of the Dutch population is vegan. In addition, the EU introduced novel food products such as insects and worms, lab-grown meat, and Bovaer for cows to reduce methane production, which might affect the human immune system. Almost one in five adolescents vape. Long-term effects are yet unknown. In the Netherlands, vapes with synthetic liquids that taste like cola, vanilla, apricot, etc., have now been forbidden . Although smoking is declining in adults, young women more frequently smoke than boys but drink less alcohol. All internal and external environmental factors may contribute to weakening or strengthening the resilience of the immune system and may therefore influence the period of pregnancy, labor, nursing, and the health of mother and child for future generations. Pregnancy Is Regulated by a Unique Complexity of the Immune System Pregnancy is a unique immunological state. The changes of the immune system in the three stages of pregnancy (very early, mid, and late stage) are meticulously timed. In the very early stage, the immune system adjusts to prevent her body from rejecting the fetus while at the same time still being strong enough to keep out foreign pathogens. In the late stage, the body is preparing for labor, which is driven by an inflammatory response. A full-term pregnancy will follow an immunological clock . Changes in this immune profile could help to predict and possibly prevent preterm labor. Studies show that pathologically-driven inflammation might trigger pre-term birth (before 37 weeks). In the Netherlands, 14.8% of the children born are preterm with 9.7% low birth weight for the duration of the pregnancy (Big2). Interestingly, in the case of a preterm child labor, the inflammatory reaction is more heated as compared to a full-term child labor. Preterm birth is an important indicator of a risk for early death, chronic and infectious diseases, sepsis, stunting, and delayed neurological and brain development. This may manifest throughout one’s lifespan. Very early birth and extreme early birth occur in only 1.5% of the Dutch baby population and are responsible for 50% of the deaths of newborn babies. The number of abortions jumped in two years in 2023 to 39,000, with most by women aged 25-34 years of age. Abortion in the Netherlands is allowed until 24 weeks of pregnancy. The number of childbirths has declined dramatically to 167,504 in 2022. That is 1.49 children per woman, with a mean age of 30.3 years. The number of women breast-feeding is also decreasing. At 6 months, women feeding breast milk lowered from 60% to hardly 30% of the young mothers. Each year, around 661 babies in the Netherlands die. Mothers dying within 42 days after labor are around 11 persons a year with an additional 5 women dying by suicide each year, and not counting women who died from cancer. Over the past years, mothers’ deaths have been increasing worldwide, with the leading cause being heart diseases and blood clots. Pregnant women with stress , depression , or anxiety , as well as obese women with gut inflammation and chronic disease, have altered immune systems and, as a consequence of malnutrition, have an altered microbiome. A weakened immune system suggests an increased risk for preeclampsia, high blood pressure, HELLP syndrome, gestational diabetes, preterm labor, and/or low birth weight. ‘Gut Feeling’ a Turmoil for Healthy Future Generations The gut presents 70-80% of the immune cells in the human body. In the mucosal layer of the intestine, neuronal cells, endocrine cells, and immune cells cooperate to manage its metabolism and bodily functioning. Recent studies in mice showed villi of the mucosal layer expanding twice its volume during pregnancy and breastfeeding, slowing food passage, improving digestion for an optimal use of available nutrition. The intestinal mucosal layer is strongly connected to various stages of pregnancy with altered gut microbiota, metabolites, and cytokines. These bioactive metabolites modulate and change the ‘innate’ and ‘adaptive’ immune system. Together, the microbial composition and the mucosal layer of the intestine determine long-term health. Mothers’ intestines influence the biodiversity of the microbiome and the resilience of the immune system, which is transmitted to the baby during pregnancy, labor, and nursing. Earlier periods in life facing hunger, extreme stress, or severe diseases may influence health during pregnancy and may transmit to the baby throughout one’s lifespan and even with intergenerational effects. Specific nutrients may have positive effects during pregnancy, labor, and nursing. Sufficient vitamin D , present in sunlight, nutrition (fish, milk products), or supplements, is a prerequisite during this precious time in life for both mother and child. For young women who wish to become pregnant, it is important to learn how to balance the immune system and the microbiome. The immune system of young women could be the most important regulator of the healthiest generations and a population’s workability and income. Author: dr. Carla Peeters First published at Brownstone Institute
The increasing number of suicides and fatal overdoses of women healthcare workers has accompanied rising sickness, disability, and women leaving the sector. The total social and economic costs of a workforce in despair are yet unknown. A shortfall of 10 million healthcare workforce (of whom 80-90% is female) is projected by the WHO for 2030 and is of critical concern. When the health of those who look out for people’s health is at risk, the whole population and economy are at risk. This is an emergency of unprecedented scale that needs attention at the highest Public Health level. Humanity and nutrition instead of medicalization as a coping strategy urgently needs to return in the healthcare sector. Alarming Warnings by Healthcare Workers in Despair Recent studies noticed death by suicide and the risk for fatal drug overdose among women in healthcare is much higher as compared with the general population (1-10). It is not only female physicians, but the risk is even higher for nurses and other healthcare workers, especially for those with the lowest-paid jobs and heaviest mental and physical workload who have been most stretched to the limits (7). Worldwide over the last several years thousands of healthcare workers have died by suicide or fatal overdose leaving family, friends, and the workplace in shock and grief. Suicide and self-harm have substantial social and economic costs (12). One death by suicide was calculated in the UK to cost the economy an average of 1.46 million pounds (13). In 2022 more than 360 nurses attempted suicide, and 72 medical professionals took their own lives in 2020 in the UK as data from the Office of National Statistics indicate. Analysis of mortality data from the US Centers for Disease Control and Prevention from 2007 to 2018 identified 2,374 suicides among nurses, 857 among doctors, and 156,141 in the general population. However, the number of death by suicide or fatal overdose is grossly underreported. The WHO reports that over 50% of suicides happen under the age of 50 years (14). To address this avoidable burden, a better understanding of effective and non-effective strategies is paramount. Even before the Covid pandemic started women in healthcare reported substantial workplace stressors (9-11, 15-16). The past four years have put additional strain on women’s health. This is especially true for those women working as front-liners and first responders in highly demanding stressful situations. Increased complexity of care, understaffing, long working hours, additional bureaucratic tasks, moral injury, diminished autonomy, lack of decision-making ability, and low-paid jobs take a burden on their health. Moreover, women routinely face tougher challenges at work and at home such as institutionalized barriers to career advancement as well as additional pressure for domestic labor by frequently being a caregiver for children and/or parents (9). In all parts of the world healthcare workers are at high risk for violence with 8-38% suffering some sort of violence form in their careers. In 2023 for the first time in history, 75,000 healthcare workers in the US went on strike (17). Women are more frequently diagnosed with burnout, major depression, Post Traumatic Stress Syndrome, ME/CFS, and Long Covid. Long Covid is more prevalent in healthcare workers (11,18-20). These diagnoses of chronic illnesses have many symptoms in common that are known to exacerbate the risk for suicidal thoughts, suicide attempts, and suicidal completion beyond occupation and established risk factors such as socioeconomic status and education (7-8,20-24). An Epidemic of Emotional Trauma and Distress Healthcare workers are trying to hide their symptoms by pushing themselves to work despite extreme pain, fatigue, memory inconsistency, exhaustion, and grief of not being able to deliver the quality of care patients need. Being overstressed and with long-term understaffing, healthcare workers hardly take time to eat a nutritious meal. Many have become undernourished, and sleep-deprived. Potential disparities in help-seeking and healthcare access might manifest in non-medical use of prescription drugs among some healthcare workers, which has implications for workers’ safety and well-being (25). Many of the medicines used by healthcare workers might be unprescribed and unnoticed (1-8, 23). Toxic Cocktails: A Danger for Women’s Health Suicides among the healthcare workforce often take place at work. The most frequently used method of suicide is overdose or poisoning (1-8). New studies suggest that most overdoses are caused by psychiatric drugs and multiple medications in their system. Co-administration of antidepressants and opioids deliberate or unplanned is common. Women are more likely to be prescribed and take medication like antidepressants and birth control pills and seem to be more sensitive and experience drug side effects than men. Pharmacokinetic interactions may increase the concentrations and severity of side effects of antidepressants (27-28). Studies demonstrate potential side effects of psychiatric drugs and opioids as insomnia, burnout, fatigue, anxiety, pain, and suicidal thoughts (21-25). The risk of opioid-involved overdose death was nearly twice as high experienced by healthcare support workers such as nursing home workers and home health aides as compared to other healthcare workers in the sector (7). The interaction and side effects of the use of multiple medicines and concentrations are mostly unknown. This is especially true for women as most drugs have been poorly studied in women. Some medicine might even have more disastrous side effects than any benefit as seems to be the case for psychotropic medicine (26). Moreover, interactions of psychotropic drugs with immunosuppressive capabilities and Covid-19 mRNA vaccines have been reported (17). Furthermore, pandemic measures that have been mandated for healthcare workers including long-term wearing of medical facemasks (with potential inhalation of toxins) and repeated Covid-19 vaccinations with women reporting more side effects than men (30-31) might have exacerbated potential risks. Recent publications repeatedly reported a global burden of absenteeism related to Covid-19 vaccine side effects which could negatively impact the strained healthcare system and jeopardize patient care (32-33). Medicalization as a Coping Strategy During the pandemic, prescription of antidepressants and use of other over-the-counter medication like acetaminophen (paracetamol) which is often advised to temper vaccine side effects, has grown substantially. Although harmless in low doses, acetaminophen has direct hepatotoxic effects when taken in overdose or a wrong combination and may cause acute liver failure. Accidental or unintentional overdose usually occurs in patients who have been fasting, or are critically ill with a concurrent illness, alcoholism, malnutrition, or have preexisting chronic liver disease (34). Acetominophen (single or combination products) is one of the most used medications in the United States with 25 billion tablets sold in 2016. It is expected that treatment of trauma ailments and increase in chronic illness will fuel the market sales from $9.8 billion in 2022 to $15.2 billion in 2033. However, after a report showed 8,700 poisonings with high rates of hospitalization and liver injury in 2019-2020 with a sharp rise among females, the Australian medicine regulator is considering restrictions on who can buy paracetamol (35). In Sweden, the sale of acetaminophen in supermarkets was banned in 2015 after they experienced an overdose hike. Increased use of over-the-counter and controlled drugs may fuel a rise in acute liver failure. Awareness of potential unintentional irreversible harm is highly needed among healthcare workers and the public, as many new drugs and vaccines have been introduced since the pandemic. Drug Theft and Diversion Job stress and occupational burnout have been associated with increased risk for opioid use disorder which in turn can increase risk for overdose. Those who prescribe or administer medication have ready access to opioids and other controlled prescription drugs. Drug theft and diversion of controlled drugs in hospitals and nursing homes appear to have accelerated worldwide, bringing healthcare workers and patients at risk (36-38). Taking prescription medicine at work, almost 100 healthcare workers have been fired in The Netherlands. Moreover, the problems with understaffing in the Dutch healthcare sector have introduced the use of falsified certificates with people from illegal drug networks entering healthcare organizations pushing the system to more errors and deficits (39). Increasing stress at work and too many night shifts in a row have contributed to a 70% increase in medicine thefts. Almost 50% of calming and sleeping pills were not delivered to patients putting them at risk for suboptimal treatment or contaminations and errors (40). Drug use may gradually become an attractive and convenient coping mechanism. Although professionals often think knowledge of the medicine may control their use, dependence may slowly develop. Many impaired healthcare workers feel guilt and despair and suffer from physical and mental problems and may be indifferent to the risk of overdose (38) A Return to Humanity in Healthcare The problem of the rise in sudden (un)intended death of healthcare workers comes against the background of increasing long-term sick leaves, permanent disabilities, and hundreds of thousands of healthcare workers leaving the sector, choosing for less stressful and better-paid jobs. This is an unprecedented sign by dedicated women for no longer willing to work in a toxic and overstressed environment with underpaid complex tasks for often severely ill patients. The healthcare system is facing increased clinical error rates and liability exposures while adversely impacting patient satisfaction and organizational reputation. This may develop into a catastrophe when Public Health Officials do not take responsibility for a highly needed change ensuring that the workforce has the tools and resources needed to turn the wheel. Hard times may turn positive when CEOs and insurance companies start to embrace the idea that quality of care and reputation starts with a healthy, fair-paid workforce, gender equity, and a working environment choosing for humanity and good nutrition. A vital well-nourished empowered healthcare workforce that is occupied to guide people to health and work will be a win for all.
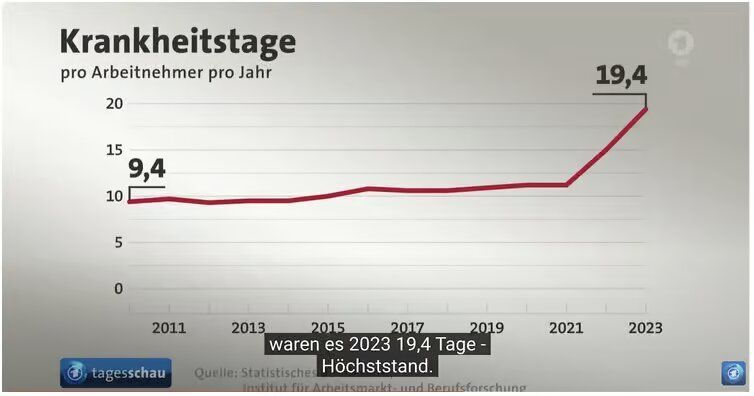
A silent disruption of population health and human potential is causing a decline in economic growth and increased poverty worldwide. The number of citizens losing trust in leaders from public-private partnerships that ruled and mandated public health and climate policies and are responsible for eroding human capital is rising. Recovery via improved investments is urgently needed. Creating healthy generations and rebuilding a flourishing economy both require trusted independent business leaders from small and medium enterprises (SMEs) who uphold finding truth and not doing harm as bedrock principles. Human Capital is the Key Driver of Economic Growth and Poverty Reduction Every business leader and politician knows that absence and poor mental health drain business. The true problem business leaders need to face is the increase in unexpected deaths at all ages, a rise in frequent and long-term sick leave, and more people experiencing lifelong disabilities. Together, they lead to a considerable loss in productivity and high costs, a rise in bankruptcy of small and medium enterprises, and an increasing number of people in poverty. Analysis of a Covid-19 Policy Score Card in the US shows a negative health effect for about 10% of the population and 30% of the civilian labor force. Business analysts are warning that this alarming negative trend is expected to continue over the next several years. Moreover, those under 25 years of age, who will make up 90% of the prime-age workforce in 2050, experienced at critical moments in the lifecycle a derailing of developments by lockdowns and school closures. This amounted to a hidden but massive loss of unmet potential with a decline in lifetime earnings as high as $21 trillion globally. The economic loss by the disastrous Covid-19 pandemic response and unneeded climate measures will exceed far beyond the $16 trillion virus . Soon, human capital will be the number one topic in risk management for business owners and investors for years to come. Skyrocketing Sickness Hits the Heart of Business Sickness hasn’t been this prevalent in decades. Independent investigators and insurance companies all point to similar observations, noticing a sharp decline in general health and well-being and an increase in sudden unexpected deaths of people in the workforce since 2021. According to Randstad 1.27 million employees miss work every day. The absenteeism rate rose to 6% in Q3 2023. The growing number of people not able to work because of long-term illness is reflected in the economic data of many countries. Moreover, mental health problems among the youth have almost doubled. Insurance companies in various EU countries, the UK, and the US have started to sound the alarm bell over the risk of recession and an increasing number of businesses that face bankruptcy due to high costs of human capital and poor performance. Switzerland Switzerland had a previous low sick leave rate of 2.4 days per year. This has changed. In the Swiss economy, absence from work due to mental illness has reached a record level and is 20% higher as compared to the previous year. Never have absences due to mental illness, burnout, post-traumatic stress syndrome, fatigue syndrome, or Long Covid syndrome been this high, with young people affected disproportionately. In the 18-24 age group, seven out of 10 people who are unable to work suffer from mental illness. This is four times higher than 25 years ago. These data reflect a structural trend. A survey by AXA Insurance among SME found that almost two-thirds are confronted with absenteeism due to mental health issues. Workplace absenteeism weighs heavily on the activities of companies. Extended employee absences can have detrimental consequences for the company’s operation. Among the most frequent repercussions are overtime and increased workload from the remaining staff (54%), costs related to recruiting additional personnel (38%), loss of production or failures in services (37%), and costs related to continuous salary payments. Germany Germany’s true economic disease, recession , includes rising sickness and declining productivity. In 2023 each employee had 19.4 days of sickness leave, almost equal to one month per employee and two times higher than in 2010. The highest increase was observed in 2022 and 2023. Filling open vacancies has become a headache for each business owner.
The news that Northern China is dealing with a mystery pneumonia outbreak in children was headlined in many news outlets worldwide. Chinese health officials failed to alert the world about a former novel coronavirus outbreak in 2003 (SARS) and 2019 (SARS-CoV-2). The WHO has stated: Chinese authorities claimed there has been no detection of any unusual or novel pathogens or unusual critical presentations so far, but only multiple known pathogens.
In many countries worldwide over the past three and a half years the health and financial situation of the population has been falling downhill in a way that has never been seen in the past decades. Trend analysis shows increasing numbers of excess mortalities in all ages and a steep rise in a decay of people’s health and workability, especially women. Pandemic measures, repeated vaccinations and a rising number of people including children and pregnant women suffering from hunger have weakened people’s immune systems.
The Netherlands has been chosen as a pilot area in the EU to be climate neutral with a transition in protein food and a transformation of healthcare into a telemedicine, data, and AI-driven connected system approach led by Public Private Partnerships. A closure of 55-70 percent of traditional farming is foreseen to be replaced by tech-driven vertical farming, gene-edited crops, edible insects, veganism, 15-minute cities and a CBDC passport covering personal health data.
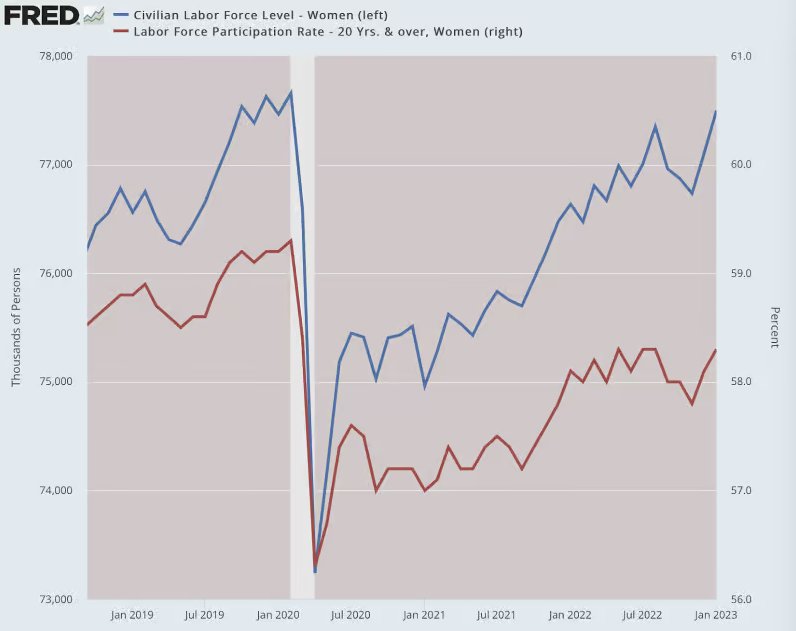
The World Health Organization, United Nations, UNICEF, non-governmental organizations and governments are all publicly promoting equity, inclusiveness and diversity. At the same time, these organizations were leading lockdowns and mandates that disadvantaged women disproportionately, especially those with a low salary, in health and income. Many of the women who lost paid work have not returned to paid work.
In an increasing number of countries all over the world chaos and despair is rising. People are more frequently ill and dying at higher rates than the past 50 years. At the same time health systems are deteriorating. We need to rethink humanness of health systems versus cold technological solutions. More than a seasonal problem The pandemic measures have accelerated public health systems to the brink of collapse. In many Western countries these systems are facing severe problems, an inferno of pressures, including staff shortages from pandemic burnout, underpaid salaries, discrimination and a cost-of-living crisis, with many health professionals leaving the workforce while the demand for care from the community is rising. The often-used explanation for the current situation in healthcare, a tripledemic after two lockdowns resulting from a surge in winter viruses (RSV, Flu and Covid-19), does not hold. Current data do not represent an outlier season. Political ideology and catastrophic leadership costs healthy years of lives The health system in the UK is collapsing because of a decade or more of underinvestment in the National Health Service and other public services. The indicators for the health service are all red. Increased ambulance times and people waiting for a hospital bed, stranded outside overflowing hospitals, have spiked since December 2022. The overstretched system , with the longest delays on record for millions of treatments for cancer and operations, has left patients in pain, people enduring unnecessary suffering, and has led to 300-500 people a week dying avoidably because of the unsolved current crisis. The roots lie in political choices made, not cold weather or a seasonal flu. On January 5, 2023 the British Prime Minister Rishi Sunak brought together the current advisors about the pressure of increasing demands. Yet, the response of top and senior managers in health services and politicians is silence , denial, disengagement, and delay, while health professionals are crying out on social media, mainstream media and the British Medical Journal to be heard. Other countries like France , Canada , and the US and The Netherlands are facing similar problems in the collapsing health system with shortness of staff and increased demands. A fall in life expectancy Excess disabilities among those aged 16-64 years , and excess mortality among all age groups is noticed in a way that has never seen before. In the US excess mortality is 40 percent up amongst working age people. Cardiac health problems and sudden deaths increased most. Undercooled and malnourished elderly people are filling hospital beds and keep them filled as they have no place to go. But also, more newborn babies and young children need hospital care. Stillbirths have skyrocketed to levels never seen before and birth rates around the world have dropped dramatically. Concern regarding a long-term increase in demand is widely spread and worrisome. A fall in life expectancy is noticed, with the greatest fall in Spain, Italy, Belgium, the US and the UK. This is of a magnitude which has not been seen since World War II. Life expectancy in the US fell by 2.7 years from 2019 to 2021 due to increased mortality and premature deaths. Covid deaths worldwide from 2020-2022 were estimated at 6,653K , which is 3.86 percent of total deaths. The number of people that survived Covid is 99.914 percent, with the highest percentage in developing countries. UK figures published this week showed that more than 650,000 deaths were registered in 2022 – 9 percent more than in 2020. Roughly 38,000 deaths involved Covid compared with more than 95,000 in 2020. Covid is one of the factors rather than the main explanation. Excess deaths in 2022 is among the worst in 50 years. A call for independent investigations is growing all over the world though they are kept on hold by Public Health ministers. The real pandemic policy More and more medical doctors and scientists are speaking out for an immediate halt of the mRNA vaccines until proven otherwise. German pathologists investigated people who died within 14 days after vaccination and observed that in certainly 30 percent of the cases but possibly 70-93 percent there was a relation. The more you vaccinate the worse the immune system gets. Recently, mandates on Covid-19 vaccines for employees in private sector NYC, healthcare workers in NYCity, and the US military have been lifted. As the tipping point of reality of the Covid pandemic policy is near, there are many within and outside Parliament and healthcare for whom questions about the coercive nature of the mandates, lockdowns and the catastrophic situation are now increasingly uncomfortable. Governor Ron DeSantis of Florida has recently called for a statewide grand jury to investigate the alleged crimes and wrongdoing surrounding the Pfizer-BioNTech and Moderna Covid-19 mRNA vaccines and the CDC. The policy of the pandemic crisis ruined lives. The immune system in all age groups has been weakened in multiple ways , while the infection fatality rate of the SARS-CoV-2 virus pre-vaccination level is 0.007 percent for people aged 0-69 years, 0.003 percent for 0-59 years of age, and 0.0003 percent for children aged 0-19 years of age. The pandemic policy is acknowledged by wrong decisions and wrong investments based on poor studies, manipulated data, assumptions, incomplete or false communications and most of all, censoring voices of medical doctors and scientists questioning the policy. In past years the genuine concern of leading politicians, public health professionals, and journalists about the health and well-being of the population are shown to be very low or at some points even absent. Accountability The health system is turned into a money driven Public Private Partnership , selling sickness , with limited interest in promoting health and well-being, let alone considering the advice of Hippocrates ‘First do not harm.’ During the past decade huge investments of tax money have been transferred to technological innovation in healthcare and even increased further over the past three years with the aim to contribute to the UN Sustainable Development Goals of the UN and Future Pandemic Preparedness , the proposed treaty of the WHO. Nevertheless, rising expenses for citizens on healthcare did not add years of a healthy life nor improved life expectancy. Even before the pandemic, the US, often referred to as having the best health system, already had the lowest life expectancy among large wealthy countries while it far outspends its peers on healthcare. CEO’s, senior managers and politicians are challenged to tackle glaring failings and accountability for current disasters which were predictable and could have been prevented. The Great resignation A recent Deloitte article reports around 70 percent of high-level executives are seriously considering quitting their jobs; 1 out of 3 executives are constantly struggling with fatigue and poor mental health, which influences firm performance. Women leaders are leaving companies at the highest rate ever. The National Rural Health Association Policy Paper reported a turnover rate of CEOs of 18-20 percent per year. Over 650 CEOs in the US left their jobs in 2022, an increase of 13 percent as compared to 2021. The complications of unstable leadership can have a significant short- and long-term impact on hospitals, quality of care and the broader community. Leadership is a vital enabler to address burnout from organizational collapsing. A need for strong and steady leadership has never been greater to prevent hospital closure and continue care, which is especially needed for hospitals in rural health . Many doctors and nurses are choosing early retirement or leaving the sector for alternative careers. Unfortunately, for people working in the frontline and supporting staff, increasing problems of burnout have been observed also. The tipping points of self-sacrifice or no longer being willing to deal with a moral conflict have passed. The monthly resignation rates in the US during 2021 were the highest in the 20-year history of the Job Openings and Labor Turnover Survey. Preliminary findings of the International Council of Nurses suggest that the Covid-19 effect is highly likely to have a significant long-term impact as it contributes to a wave of post-traumatic stress disorder, depression, and anxiety. Even if only 10-15 percent of the current nursing population quits because of Covid-19, the effect there could be a potential shortfall of 14 million by 2030. which is the equivalent of half the current nursing workforce. Prior to the Covid-19 pandemic severe burnout was typically found in 20-40 percent of the healthcare workers. European Junior Doctors (with 300,000 junior doctors) said in a press release : “Healthcare in Europe is at a precipice. The situation is not new, it was predictable and preventable.” Alarming rates of burnout and other mental problems have resulted in many junior doctors leaving and considering leaving the workforce. Burnout , depression and anxiety are harmful for the healthcare system, healthcare workers , and patients and are characterized by emotional exhaustion, depersonalization and diminished personal achievement. Risk factors have been exacerbated during the pandemic. Also symptoms of Long Covid were found to be increased among healthcare workers as compared to people working in other sectors, resulting in an urgent need for intervention. The overall long-term effects of the Covid measures on people working in the healthcare sector are yet unknown. The symptoms that are contributing to Long Covid and burnout, depression and anxiety could be a result of pandemic measures and masking in particular. A crisis to speed the transformation to ‘smart’ hospitals The collapsing health system enables politicians and healthcare leaders to suggest a range of private market solutions to the healthcare crisis by technology and to contribute to the Sustainable Development Goals to be realized in 2030, as quick fixes for healthcare workers and shortage of beds won’t be realistic. Burned-out doctors and nurses are being replaced by outsourcing at considerable cost . This will speed up the transformation to ‘smart’ hospitals advised by consultancies like McKinsey , KPMG and Philips NV , using AI, robotics, 3D printing, genomics, telemedicine, and precision medicine. 5G technology is introduced to realize Hospital Intelligent Twins for all scenario intelligence healthcare which is already operating in Guangdong, China. These policies are focused on more money, technology, digitalization and robotization, preparing a revolution to transhumanism and a digital health passport with all information of each citizen available in a central system. The experience with the Covid pandemic has shown transhumanism is a ‘ utopia ’ that can only ever materialize in a dystopia embracing the limits of the world as well as those of the human condition. The way out will be the human factor, not Big Data . Humanity returns in the center of healthcare The loss of trust in government and health systems is bone deep for those who have lost loved ones, have become disabled, and lost their income. On Saturday January 7th 6 BBC buildings were covered with posters, stickers and pictures of people who were believed to be injured or killed by the vaccine: “BBC is the virus.” Heartbreaking situations urgently need support and care. Interventions are needed to prevent similar situations. Unfortunately, most of the interventions often suggested lack evaluation or evidence to support them. Experienced leaders in change are urgently needed to restore openness and transparency, resilience, and support the healing of people in sickness leaves and prevent more people leaving healthcare. As recently proposed by DeSantis, mask and vaccine mandates should be permanently banned as well as the controversial Covid-19 Hospital Immunity protocol. The highest priority is a focus on the well-being of all employees, and safe and cost-effective treatments including nutrition and lifestyle interventions strengthening the immune system to support all people in choices for a healthy life. Employees with natural immunity fired during the pandemic should be hired back. Processes need to be simplified and focus on human-centered care. Leaders of change in healthcare live the principles of universal public health coverage funded by taxation, being responsible and committed, and are not afraid to speak out, guiding organizations into empowering environments embedding a relationship of trust in the doctor-patient relation at the core of Medicine . Patients will be given optimal information of what healthcare workers know, so they can make informed choices . This will lead to positive change paving the road to a healthy economy making safe and effective, equitable, and human-centered healthcare affordable for all a reality. Author: dr. Carla Peeters First published at Brownstone Institute



